HRV (Heart Rate Variability) is the measurement of the variation in time (in milliseconds) between two consecutive heartbeats.
A high HRV reflects the autonomic nervous system's ability to switch flexibly between "stress" mode (sympathetic) and "recovery" mode (parasympathetic). Therefore, HRV is an excellent indicator of the overall stress level our body is facing.
There is also a direct link between HRV, sleep quality, and depression [1] [2]. HRV influences sleep, and sleep influences HRV. Indeed, better sleep quality increases HRV and lowers the resting heart rate the following day. Conversely, a high HRV improves sleep quality—especially deep sleep—the following night.
Several studies also link HRV to depression; individuals experiencing depression often have low HRV. A low HRV is frequently a sign of a "loss of vagal flexibility." Essentially, the body stays stuck in "survival" mode (sympathetic) and can no longer activate the "brake" (parasympathetic) to soothe itself. This explains why one might feel less depressed when HRV improves: the body has regained its physiological ability to calm down. It is, therefore, a strong indicator of resilience [3].
You don’t need medical-grade equipment to monitor your HRV. It can be measured with almost any modern smartwatch or fitness tracker, such as Apple Watch, Fitbit, Samsung Galaxy Watch, Garmin, or Whoop for example.
This is anecdotal, but I experienced it recently. I lately implemented a system to increase my HRV. I am 36 years old, and I went from approximately 50 ms to 70 ms in one week. And indeed, although I don't necessarily feel like I'm sleeping better, I am slightly less tired and, above all, less depressed.
It remains to be seen if this trend continues over time and if I can maintain this value, which I suspect will not be an easy task.
So, how do you increase your HRV in practice?
Even if you are thin and looking to gain weight, do not force yourself to overeat. This will lower your HRV, which in turn lowers your sleep quality and, eventually, reduces your digestive capacity. It becomes a vicious cycle of metabolic stress. If the body spends the night digesting, it isn't spending the night repairing the nervous system.
You can create a virtuous cycle: eating slightly below your maximum digestive capacity increases HRV, which improves sleep quality and, ultimately, boosts your digestive capacity the next day.
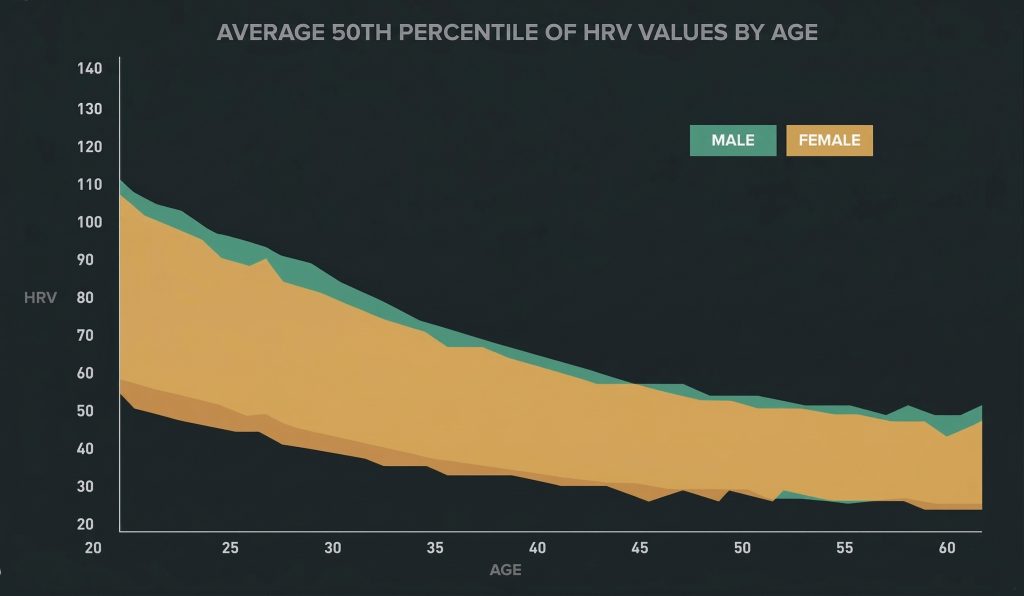
HRV is a reliable indicator of physical stress and is very useful for monitoring your general health. To give you an idea of typical values, here is a chart showing HRV relative to age.
In people with Empty Nose Syndrome (ENS), the sensation of airflow is often absent or altered, largely due to a loss of wall shear stress (WSS), the mechanical force exerted by air as it flows along the nasal walls, which is sensed by receptors in the mucosa. This stress depends not only on airflow rate but also on the geometry of the nasal cavity.
During sleep, the flow rate naturally decreases. While a person at rest during the day typically breathes between 8 and 15 L/min, airflow can drop to just 4–6 L/min during deep sleep. This leads to a decrease in airflow velocity through the nasal passages.
Wall shear stress is directly related to the velocity of airflow in contact with the nasal mucosa. When airflow drops as it does at night the flow slows down, resulting in a dramatic drop in WSS and thus in sensory stimulation.
| 15 l/min | 6 l/min | Percentage reduction | |
| Pressure loss (Pa) | 6 | 1.5 | 75 |
| Mean WSS (Pa) | 2,43E-03 | 7,09E-04 | 71 |
I performed two CFD simulations on my own nasal cavity: one at 15 L/min and another at 6 L/min. The results show a 75% reduction in pressure loss (nasal resistance) and a 71% drop in WSS.


On the left: WSS at 15 L/min (daytime), on the right: 6 L/min (nighttime). It’s clearly visible that WSS values are much lower on the right, reflecting the reduced airflow during sleep.
Normally, the nasal turbinates actively adjust to changing flow rates: they swell or shrink (via vasodilatation or vasoconstriction) to modulate the cross-sectional area through which air flows. When airflow decreases, turbinates can swell to increase resistance, helping maintain airflow velocity and thus WSS.
But in ENS, part or all of the turbinates have been surgically removed. This adaptive capacity is lost. The nasal cross-section remains fixed and often too wide for the low airflow of nighttime breathing. As a result, airflow slows, becomes less turbulent, and fails to stimulate the mucosa. This worsens the paradoxical sensation of nasal obstruction and dryness.
In this context, it makes sense to consider nasal volume adaptation based not only on the commonly used 15 L/min daytime flow (used in CFD simulations), but also on a more realistic nighttime flow of 4–6 L/min. This would help define a nasal cross-section that maintains sufficient WSS during sleep when symptoms are often most severe.
Practically, nasal implants or prostheses could be designed for nighttime airflow.
In the previous article I showed you a device for visualize your breathing. In this article I will show you how to use it as a sleep breathing recorder in order to detect hypopnea and apnea.
For it, I have just connected the microcontroller arduino to the PC with a USB cable and use two software. One for recorded the breathing curve and one for read it. The first soft is coolTerm it recorded the pressure data in a .csv file. The second is a web app called chart studio ploty which can read easily and quickly the .csv file. You can also read the .csv file with Excel but it is slow to open.

This is the breathing curve in chart studio ploty, you can zoom and navigate in order to see the entirely night sleep and detect apnea events. The y axis (vertical) represent the pressure in Pascal (pa), the x axis represent the time but the unit is not second nor millisecond. However, you can estimate the time by the frequency of breathing, at night we breathe around 10 time per minute, so one breath every 6 second.

The main problem is that you should count every apnea manually, there is no algorithm to do that. In sleep clinic they use a dedicated software to count apnea and hypopnea, they also have others data like brain waves, sound, oxygen saturation and others things. Maybe at home you can complete this device with an oxygen saturation recorder.
That's it for this article ...
Empty Nose Syndrome can affect your sleep in some ways.
Some people wake up after one or two hours because the nose becomes dry.
But I think that the first reason ENS affects our sleep is because it creates central sleep apnea.
It is a respiratory problem which occurs when a person who suffers from this condition is sleeping. The respiratory reflex who is commanded by the brain is reduced or is completely stopped when the person falls asleep. In general this problem is due to a brain problem (brain tumor, cerebral vascular accident ..) or heart problems.
In ENS case the nasal turbinates are completely or partially cut. Then, the mucosa doesn't correctly react to the air entering in the nasal cavity and this lack of sensation reduces the respiratory reflex. The brain is no longer informed about the breathing and it creates a disorganization.
Dr Houser has published some years ago an interesting paper about the link between ENS and Central Sleep Apnea.
Apparently there are two sensors which inform the brain about the breathing.
Mechanical sensors feel the pressure created by the air passage in the nasal cavity. That's interesting to note that the narrower the nasal passage is, the higher is the velocity and the pressure.
The temperature sensors feel the difference between the temperature of the mucosa and the temperature of the inhaled air. It also works with the phenomenon of evaporation of the mucus. When you inhale, the air is normally dryer than your mucosa, so the thin mucus film is evaporated at the air contact. This evaporation cools the mucosa by the changing state of the water (mucus), from liquid to gas.
That's why in order to have better feeling we should find a way to increase the pressure, the temperature of the mucosa and the moisture.
Cartilage implant for improving the nasal air flux, the humidity and the temperature of the mucosa
In other posts I will speak about the solutions that don't require surgery. But of course, an implant can also be a good solution.
While in the previous post I explained why ENS can affect the sleep, in this post I will explain how a CPAP machine can help you to sleep better.
There are two types of machines, the CPAP which is normally designed for obstructive sleep apnea and servo ventilation which is designed for central sleep apnea.
A CPAP is a machine which sends pressurized air at constant pressure, generally between 4 to 20 cmH2O through a mask. The air expands the upper airways in order to prevent the obstructive apnea. Of course, this machine can also help you if in addition to ENS you suffer from obstructive sleep apnea which is more common than you think ( 40% of men older than 40 years). But this machine can also help you to breath at night. The pressure and the velocity of the air increases the airflow sensation which is good for respiratory reflex and can decrease the central sleep apnea. In addition, you can choose a CPAP with a humidifier bloc, which can humidify your nose well with correct settings and a heating pipe.
A servo ventilation works differently: there are two levels of pressure, one for the expiratory pressure and the second for the inspiratory pressure. There are two other settings, the breath per minute (BPM) and the inspiration time, which is often between 1,5s and 2s. This machine litterally breathes for you. But a breath to be initiated, the difference between the two levels of pressure should be high enough, more than 10 cmH2O which is not comfortable. Moreover, this machine is difficult to obtain. You need a polysomnography record which shows multiple central apnea.
Then if you have sleep problem related to ENS, you can try CPAP machine first with a good humidifier bloc. I also advise you to use a nasal mask like on the picture below. I feel that it's better to retain humidity in the nose.

If CPAP does not improve your sleep, you can consider the servo ventilation. But I have personally never tolerated it and even with high difference of pressure it is not able to maintain my oxygen saturation. I wake up after 2 or 3 minutes due to the lack of breathing airflow.